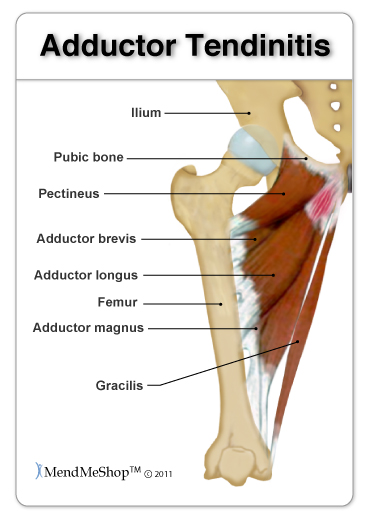
The hip adductor muscles help bring your legs together and rotate your hip inwards. The short adductors include the pectineus, adductor brevis, and adductor longus, and the long adductors include the adductor magnus and gracilis. These muscles start at your pubic bone where the crease of your inner thigh meets your body and move down your thigh bone to the inside of your knee. At the end of these muscles are tendons, which are tough, fibrous tissues that connect muscles to bones.
Groin injuries comprise 2 - 5% of all sports injuries; adductor tendinitis and tendinopathy are among the most common causes of groin pain in athletes. The adductor longus is responsible for 62% of groin injuries, and tends to be the most prone to injury, followed by the gracilis muscle. This injury is problematic among athletes especially runners and professional dancers, as both activities stress the adductor tendon quite heavily.
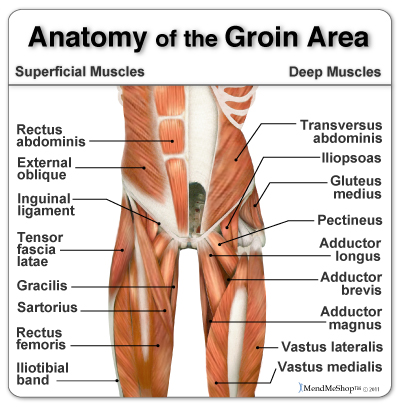
This can be classified into 3 grades of pull or strain severity:
Minor - Grade 1 involves stretching of your muscles which results in slightly pulled muscles or very small tears in your muscles. You will generally feel mild cramping which will be a little tender or uncomfortable, but will involve no swelling or no loss of strength.
Moderate - Grade 2 are more painful and involve a partial tearing of the tissue fibers in your muscle, tendon, or at the tendon attachment to your bone. You will generally experience some pain, along with swelling, decreased range of motion and strength, as well as difficulty walking or running. Your muscles will often be painful when you touch them.
Severe - Grade 3 means a complete tear (rupture) of your muscle fibers generally at your muscle/tendon and bone attachment; it is very painful and less frequent than the others. You will tend to experience a burning or stabbing pain, a lot of swelling and minimal strength, which may prevent you from walking without assistance or make it impossible for you to run. Bruising in the injured area is common a few days after the accident. This type of pull or strain may require a surgical repair.
If you do not allow your tendons and muscles to heal properly, previous adductor injuries will build upon each other. The inability of your tendon to repair itself encourages micro-tears to accumulate faster than they can heal, increasing the breakdown of your tissue and reinforcing your pain and disability. The majority of adductor strains are grade 1 or 2 strains that involve partial tears, where your adductor tendon and muscle meet.
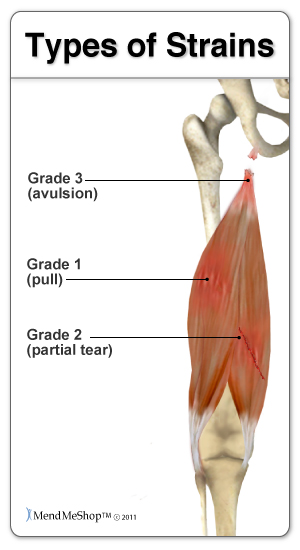
Groin Strain is a common term, often referring to Adductor Tendinopathy, Adductor Tendonitis, Adductor Tendinosis, Groin Tendonitis, Groin Tendinopathy, Groin Tendinitis and/or Groin Tendinosis
If you are suffering from Adductor Tendonitis you may have pain if you touch the area where tendon attaches in the pelvis. A sharp, stabbing pain may be experienced in your groin and inner thigh area. Pain levels raise when squeezing your legs together or when moving your affected leg away from the mid-line of the body. You may have aching or stiffness in the groin that increases with rest following or after a physically demanding activity. The pain in the groin and hip area develops gradually overtime. If you have a chronic injury, you may feel more of a dull ache> that lasts for long periods of time.
You may experience stiffness and decreased range of motion (ROM) in your hip joint as a result of injury in your short adductor muscles. This will make it more difficult to bend and rotate your hip and knee. If you have tightness, pain and/or tenderness while doing this, you are likely suffering from a damaged adductor. You may also feel tightness in your lower abdominal, spine and hip region. This is often more prevalent on the left than right side, however it is really dependent on your injury.
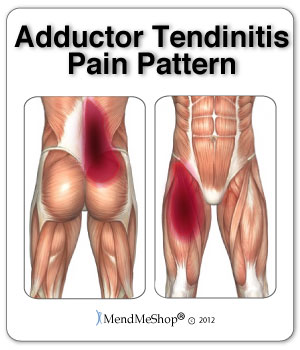
If the condition persists and becomes chronic Adductor tendonitis, you may experience pain symptoms that increase during activity. Your range of motion will be affected - so much so that you may limp as a result of the pain.
Weakness of your adductor muscles can also be experienced as a result of adductor tendinitis or tendinopathy. This along with your other symptoms may make it difficult for you to walk or run and can result in you walking with a limp.
Occasionally, bruising (broken blood vessels) in your groin area or over your adductor muscles may appear a few days after your injury. This may be in one spot or can span from your groin to your knees.

Warmth, redness and/or a tender lump may accompany adductor tendinosis and severe cases of tendinitis. Swelling in your adductor muscles is a result of your tissues becoming inflamed; inflammation normally occurs with a more acute adductor strain and/or adductor tendinitis. Chronic cases will typically have little to inflammation.
The most common cause of tendon inflammation is overuse of your area. It results from repetitive stress placed on your adductor muscles and tendons during active sports (especially when running, kicking, twisting, or side-stepping). Result of a sudden fall or direct hit, and/or overexerting yourself in everyday activities that involve twisting or lifting heavy objects while bending or running on an unstable surface (like grass or mud). Sports such as football, hockey and athletics (particularly sprinters, hurdlers, and long jumpers), skiing, horse riding and gymnastics, all commonly have Adductor tendonitis injuries.
Adductor tendinitis can also stem from alignment issues and leg length discrepancies, which affect the way you walk. It can also be caused by incorrect sport-specific motions, as well as strength differences in your muscles, lack of exercise and obesity, age-related weaknesses and/or degeneration, and genetics.
Avoid doing too much too soon - decrease, modify and/or avoid any activities that cause pain and irritation.
Stabilize your groin, pelvis and hip area, build your core strength with light weights, exercise bands and balls, core balance training, and exercises to develop strength, speed and agility, such as jumping or bounding. Yoga, Tao chi, or a daily stretching routine will also help keep your muscles and joints supple, and will increase your range of motion. Combine these with regular low-impact exercise and healthy diet.
Always warm up and cool down your muscles, learn the proper form and techniques to prevent injuries, and utilize any available mobility supports (braces, taping, orthotics, canes) to help alleviate undue stress and improve your function.

Groin pain is often difficult to diagnose, especially when chronic; however, adductor tendinitis is among the most frequent and easily identified groin related pain. To help your doctor achieve a proper diagnosis, he/she will begin with a medical history about you, your current condition and symptoms. He/she will inquire about the intensity of your present pain, the duration of your symptoms and the limitations you are experiencing. Details about the injury, when it started, and whether or not you have ever had treatments for this or a similar condition in the past, will be very helpful in assessing your injury.
A physical examination will be performed to determine if you have any signs of adductor tendinitis or tendinopathy. Your doctor will look and feel the muscles, bones and other soft tissue in and around your pelvis and groin area (near and/or including your genital area) as well as your hip, spine, and lower body to evaluate sameness, recognize differences and identify pain and tenderness. This will help to discover any abnormalities, such as mild or severe inflammation, fluid, bruising, bone or tissue deformity. He/she may ask you to complete a series of hip and leg movements to see what motions cause pain, weakness or instability, such as contracting your adductor muscles against resistance. This will help to determine the location of your injury and test for the grade of your adductor injury. He/she will also check the way you walk (gait) to determine if you have any adductor or other muscle weakness.
X-rays will provide a two-dimensional image of the overall structure of your pelvis and groin. They are helpful in identifying pelvis instability, fractures, abnormal bone shapes (bone spurs or bone cysts, wear and tear on the joints) and/or other groin or hip problems.
Isotope Bone Scans are used to identify bone abnormalities, such as a tear, inflammation, fracture or infection of the pubic bone. It will also identify whether other groin conditions are present (osteitis pubis, sports hernia, fractures).
MRIs (magnetic resonance imaging) will provide more detailed information and will help to evaluate the soft tissues in and around your groin and pelvis (muscles, tendons, ligaments, fascia, and other connective tissues). It can identify ligament or tendon damage, and can help to determine the extent of your injury, the grade of your tear or inflammation, as well as other associated groin conditions.
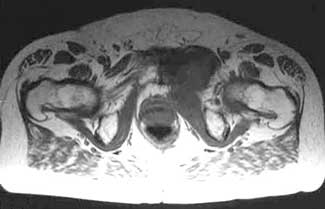
Diagnostic ultrasound (Ultrasonography) or CT scans (computerized tomography) can be used to provide a more thorough 2 or 3-dimensional assessment of the soft tissues, organs and bones in and around your groin and pelvis. Ultrasound is useful for diagnosing and locating muscle and tendon tears, but not tendinopathy.
Initial treatment should focus on resting your leg/hip/groin and reducing the inflammation to help relieve pain. Do not train through the pain. It may be necessary to stop work and activity for a few weeks or more. The good news is that most cases of Adductor Tendinitis will heal with simple home conservative treatments and surgery is often not needed! First you need to stop the activity that is causing your pain and rest your hip and groin.
Product Advisors are available 9:00 am to 5:00 pm Eastern Standard Time Monday to Friday.
I want to learn more about Post-Surgery Recovery
I want to learn more about TShellz Wrap® Circulatory Boost
I want to learn more about Ice & Heat: Which Is Better For Treatment?
I want to learn more about Tendonitis Treatments
I want to learn more about Tendonitis Surgery
During your recovery, you will probably have to modify and/or eliminate any activities that cause pain or discomfort at the location of your soft tissue injury until the pain and inflammation settle. The more diligent you are with your treatment and rehabilitation, the faster you will see successful results!
Please be aware that this information is neither intended nor implied to be a substitute for professional medical advice. CALL YOUR HEALTHCARE PROVIDER IMMEDIATELY IF YOU THINK YOU MAY HAVE A MEDICAL EMERGENCY. Always seek the advice of your physician or other qualified health provider before using any of our outstanding products to make sure they are right for you and your condition or if you have any questions regarding a medical condition. Always see your doctor for a proper diagnosis as there are often many injuries and conditions (some very serious) that could be the cause of your pain.
© 2025 In.Genu Design Group, Inc. Contact Us